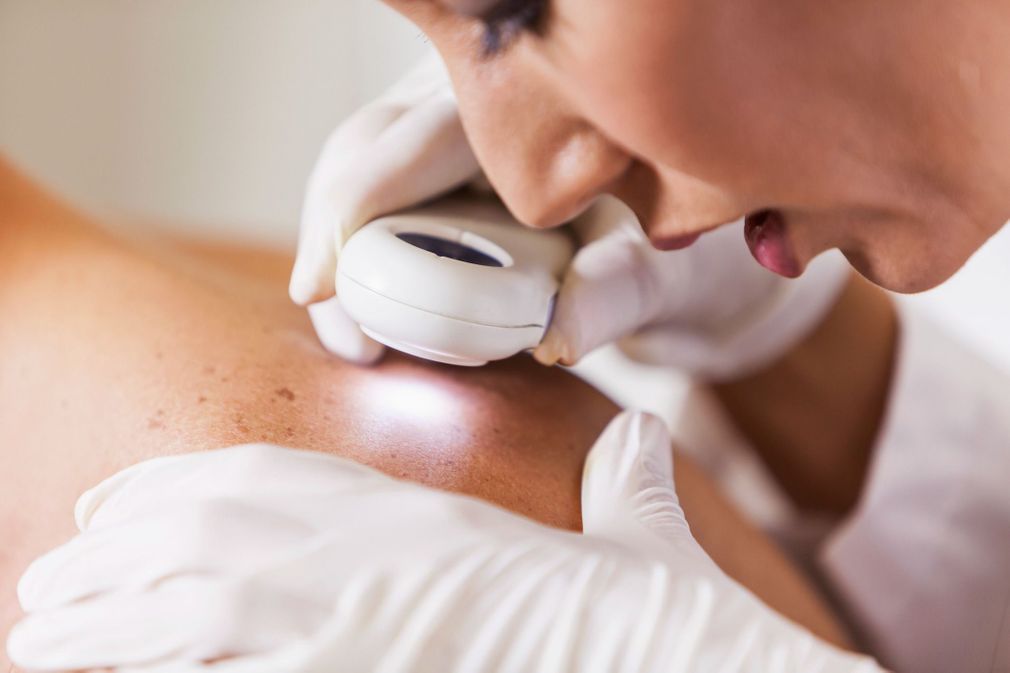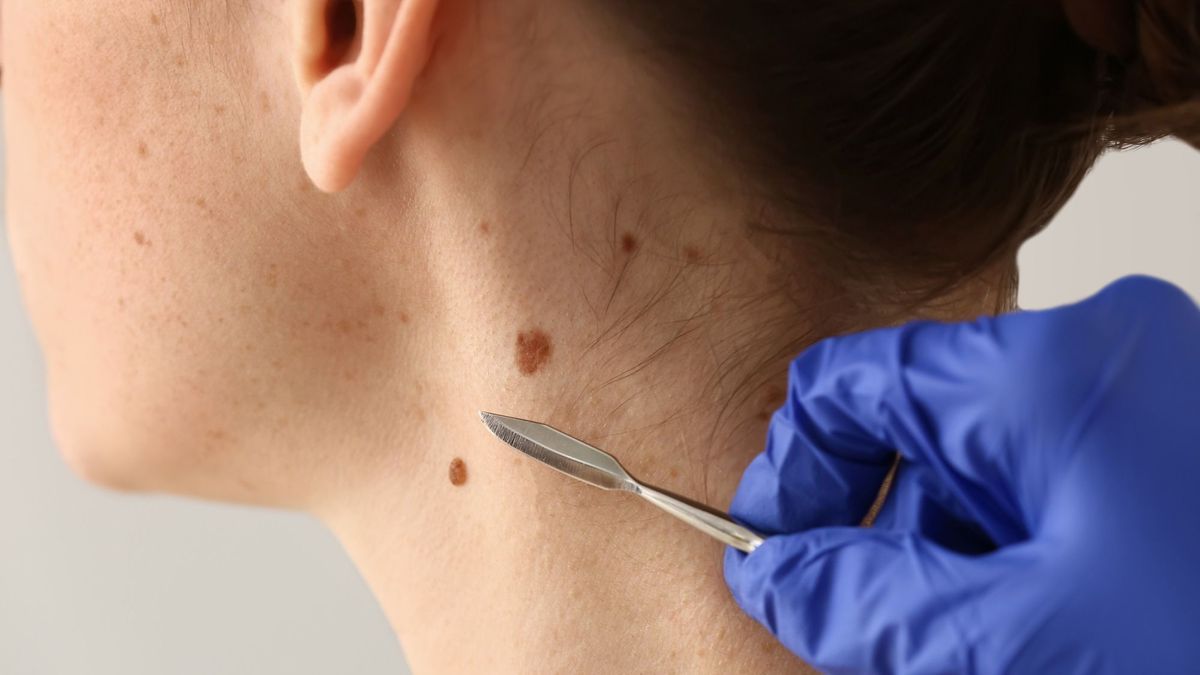
An excision is a surgery which consists of removing an anomaly, a tumor, a part of an organ or an entire organ. Its aim is to make a diagnosis or to treat. Excision is a synonym for ablation but this term is used more in dermatological surgery. Here is everything you need to know about surgical excision in dermatology, with Dr Laura Chanel, surgeon specializing in reconstructive and aesthetic plastic surgery.
In dermatology, excision consists of surgically removing lesions from the skin. Concretely, the surgeon cuts (excises) a more or less wide or deep part of the skin to treat an anomaly or resect an excrescence.
The skin lesions concerned can be benign (mole, cyst, etc.), malignant (carcinoma, melanoma, etc.) or suspected of being malignant. Surgical excision can be performed on any area of the body since the skin is the largest organ in the body and a lesion can occur anywhere.
Who performs excision?
Surgical excision is carried out either by a dermatologist or by a surgeon specializing in reconstructive plastic surgery. The dermatologist is generally responsible for removing malignant lesions or lesions at risk of cancer. The surgeon specializing in reconstructive plastic surgery performs excisions to remove malignant or potentially malignant skin lesions, but also benign ones (the patient is bothered by the lesion from a functional point of view or is self-conscious because it is unsightly).
In which cases should an excision be carried out?
Surgical excision is planned in two cases:
- To remove malignant lesions. This concerns skin cancers such as carcinomas and melanomas. “These patients that I operate on are generally referred by dermatologists after a biopsy has made the diagnosis of cancer. But I may also be required to do the biopsy myself and then see if additional surgery is necessary.”explains Dr. Chanel.
- To remove benign lesions. “These may be benign lesions that can develop into cancer, such as actinic keratosis, or lesions that are unsightly or that bother the patient from a functional point of view. The most common example being a mole placed on a bra strap.indicates the surgeon.
You should know that radical surgical excision is the main treatment for cancerous skin tumors. She “makes it possible to achieve a definitive cure rate of around 99% for skin carcinomas”reports the French Society of Dermatology on its site.
The use of excision to remove a benign skin abnormality should be discussed with the doctor. Indeed, the possible risks of this surgery must be mentioned, in particular the expected scarring result. The objective is to obtain a residual scar that is less visible than the removed lesion.
How does an excision take place?
The preoperative consultation
A consultation with the dermatologist or surgeon specializing in reconstructive plastic surgery is necessary before the procedure. It allows the doctor to precisely define the nature of his surgery (size and shape of skin to be excised, type of anesthesia, etc.) and to inform the patient about this type of intervention. This appointment also allows the doctor to learn more about the patient’s medical history and possibly current treatments. Finally, this prior consultation gives the patient time to assimilate all the information received by the doctor before D-Day since it takes place approximately 10 days before the procedure. He can thus confirm his surgical appointment or cancel it knowingly.
Anesthesia
The type of anesthesia chosen will depend on the size of the lesion to be removed and its location. The procedure can be carried out under simple local anesthesia, sedation or general anesthesia.
In the case of local anesthesia, the anesthetic product is injected into the skin to numb the region affected by the excision. In the vast majority of cases, the product used is adrenalinated xylocaine. This relieves the pain and tightens the small vessels to reduce bleeding. This anesthesia may possibly be preceded by local preparatory anesthesia using an anesthetic cream or patch applied two hours before the procedure. Preparatory anesthesia aims above all to avoid the pain caused by the injection of the anesthetic. “I always prescribe granulated arnica to my patients, to take before the procedure. This helps limit the appearance of postoperative bruising.says Dr Chanel.
Excision
Once the area is anesthetized, the dermatologist or surgeon can begin surgical excision. To do this, he uses a scalpel and an electrical device allowing the coagulation of small vessels. In the case where a skin tumor is operated on, the objective is to remove it in its entirety. The size of the excision must be larger than the lesion to be sure that all of the tumor cells have been removed. If the tumor is malignant, the dermatologist or surgeon must remove a healthy area around the tumor (the safety margin) the size of which varies depending on the nature of the cancer. This safety margin is 4 mm for a non-invasive basal cell carcinoma and can go up to 2 cm for a melanoma.
Once the lesion is removed, the doctor sutures the edges, bringing them together. In other words, it closes the skin. But this technique is not possible for certain locations such as the angle of the eye, the tip or the side of the nose because this would risk deforming the area and the orifices surrounding it (mouth, eye, nostril). The dermatologist or surgeon must therefore practice surgical techniques using skin flaps. This involves mobilizing skin from other parts of the body. For the face, these flaps of skin are taken from the cheek.
For simple excisions, the surgical procedure ends with the placement of stitches. The thread used is absorbed into the skin on its own in the deep part (the dermis). The thread used for the superficial part is a non-absorbable thread which will have to be removed on average 8 to 15 days later depending on the location of the intervention. “If the excision was carried out on the face, the stitches are removed one week after the procedure. If it was performed on another part of the body, the stitches are removed 15 days after the procedure.points out the surgeon.
The surgical aftermath
After the suture, the doctor makes a dressing before prescribing post-operative care. “I prescribe a healing cream to my patients, which they must apply every day for a month. Then, I advise them to apply a silicone-based cream for three months. Exposure of the scar to the sun should be avoided for one year because the scar evolves for one year after the operation. A scar that is not mature and tans will never tan!”, warns Dr. Chanel. Finally, it is advisable to avoid putting tension on the scar for 15 days (carrying heavy loads, sports, etc.) and to avoid places where it is hot and humid (saunas, swimming, etc.) also for 15 days. .
In the event of a malignant tumor or suspected of being malignant, the piece of skin taken is sent to a specialized anatomo-pathology laboratory to be examined under a microscope. This examination makes it possible to verify the nature of the lesion but also to verify that the excision has been sufficient, that is to say that the resection margins are well located in healthy tissue. If this is not the case, you will have to operate again.
Special case: the shaving technique
Shaving is a surgical excision technique which can constitute an alternative to traditional excision. It is generally used for the most superficial lesions, such as benign moles. Carried out under local anesthesia, shaving consists of shaving the mole on the surface using a scalpel. The advantage of this technique is that it does not leave a scar. On the other hand, there is a risk of regrowth of the mole. Shaving can also be advantageous in areas that are difficult to repair such as the angle of the eye, but also in areas where the suture could be long (areas of great muscular tension).
What are the potential complications ?
According to a national study carried out by French dermatologists, the rate of complications following surgical excisions is 5%. The complications most often reported were benign: vagal discomfort during the procedure, bleeding from the surgical wound after the procedure (particularly in patients on anticoagulants), post-operative infections (benign in the majority of cases).
If the patient presents unusual symptoms following the procedure such as swelling of the area with redness, bleeding or pain with discharge of pus, a consultation with a doctor is necessary.
What support ?
Excisions of malignant tumors or tumors with a high risk of malignancy are partly covered by Social Security. All or part of the remainder can be reimbursed by the mutual insurance company.
Excisions for aesthetic purposes at the patient’s request are not covered by Social Security.