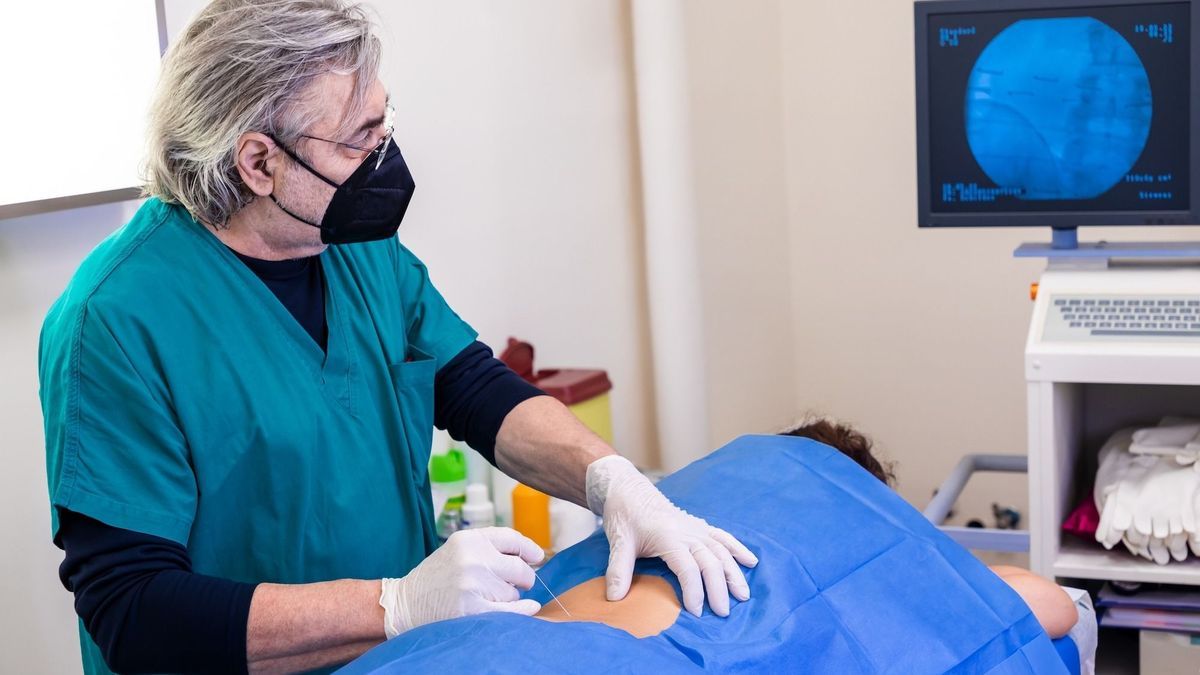
Lumbar infiltrations consist of injecting an active ingredient (most often an anti-inflammatory corticosteroid) into a structure of the spinal column, with the aim of relieving lower back pain, sciatica and persistent cruralgia. Carried out under clinical or radiological control, this invasive medical procedure is very precise but its effectiveness remains variable. Update with Dr Gilles Avenel, rheumatologist at Rouen University Hospital (Rouennais Spine Institute) and president of the Spine section of the French Society of Rheumatology (SFR).
What is a lumbar infiltration?
Lumbar infiltration consists of injecting a treatment into one of the anatomical structures of the spine in order to locally reduce painful phenomena. “The injection is done in the spine at the level of the epidural space, the posterior joints or more rarely in the foraminal or intra-discal area.explains Dr. Gilles Avenel, rheumatologist at Rouen University Hospital (Rouennais Spine Institute) and president of the Spine section of the French Society of Rheumatology (SFR).
It can be carried out by a clinician (rheumatologist, orthopedist, sports doctor, etc.) or by a radiologist and then takes place under radiological or scannographic control: this guidance helps to reach the area to be treated. The infiltration thus allows an effect on the very site of the pain, while maintaining a low general diffusion, which also makes it possible to limit the side effects linked to the anti-inflammatory treatment. The therapeutic effect obtained by lumbar infiltration is transient: it generally lasts a few months and must be associated with more global treatment with rehabilitation. Furthermore, the infiltration must be repeated regularly, up to 2 to 3 times per year depending on its effectiveness.
Indications: for which pathologies is it recommended?
Lumbar infiltration can be offered to treat certain painful pathologies. “This mainly concerns sciatic or crural radiculalgia (Editor’s note: compression of a nerve root) caused by a herniated disc or degenerative lumbar stenosis (narrowing of the vertebral canal).”, observes the specialist. Infiltration is thus offered to patients suffering for several weeks, not calmed by rest and drug treatments. “It can also be recommended for patients with radiculalgia secondary to ductal narrowing, responsible for neurogenic claudication (cruralgia or sciatica occurring when walking and improving when stopping).”.
More rarely, they are used for the treatment of chronic lower back pain, when a specific anatomical structure is suspected as the main source of pain. This is then a posterior joint infiltration.
“Exceptionally, intra-discal infiltrations are offered, in chronic low back pain patients presenting specific anomalies such as so-called “MODIC I” discopathies on MRI. This type of treatment is offered after failure of usual treatments, in centers specializing in the management of chronic low back pain and after a multidisciplinary consultation meeting”adds Dr Gilles Avenel.
The prescription for lumbar infiltrations is often made by a rheumatologist, a sports doctor, an orthopedic surgeon, a neurosurgeon or a general practitioner.
What are the different types of infiltration?
Depending on the area injected, we distinguish:
- Epidural infiltration (interlaminar, interspinous or via the sacrococcygeal hiatus), often used in radiculalgia (herniated disc, narrowed lumbar canal);
- Foraminal infiltration which consists of infiltrating the canal through which the nerve root exits. “This type of infiltration is, however, practiced less and less because it carries a greater risk of neurological complications”;
- Posterior joint infiltration when these joints are suspected of being the cause of low back pain;
- Intra-disc infiltration (in cases of inflammatory disc disease).
What products are injected?
Most of the time, the product used is an anti-inflammatory corticosteroid. “Local anesthetics can sometimes be combined to improve comfort during the procedure or increase the effect of the corticosteroid., adds the rheumatologist. Finally, certain products are under development and must still be evaluated, such as platelet-rich plasma (PRP) or intradiscal gels.
What are the benefits of infiltration?
The infiltration has a symptomatic effect on pain and provides relief by reducing the risk of adverse effects linked to taking systemic treatment (oral, subcutaneous, intravenous or intramuscular). Unfortunately, the observed benefits are not constant from one individual to another.
Which doctor should you consult?
Spinal infiltrations can be carried out under radiographic/CT control or be carried out directly by a doctor in the office, without control imaging. However, they are most often carried out by a rheumatologist or a sports doctor.
What to think about before the procedure?
Several scenarios need to be mentioned to your doctor, before scheduling the infiltration, so that the necessary precautions can be taken:
- Report any medication known to cause bleeding (or “thinning the blood”): anti-vitamin K anticoagulants (Sintrom, Previscan, etc.), use of Heparin, Coumadin; antiplatelet drug treatment or aspirin derivatives (Aspégic, Kardégic, products such as Plavix, Ticlid, etc.);
- Report your allergies if you tend to feel unwell;
- If you are pregnant or breastfeeding;
- If you have diabetes (this is not a formal contraindication, but increased monitoring of blood sugar levels must take place in the following days);
- In case of fever or recent infection: the infiltration will probably be postponed.
How does lumbar spine infiltration take place in practice?
On the day of the exam, be sure to bring:
- The prescription or letter from your doctor.
- Your radiological file (x-rays, ultrasounds, scanners, MRI, etc.).
- Your usual treatment prescription.
- Your health insurance card, mutual insurance card, as well as an identity document.
- The product necessary for the administration of the infiltration.
Before going to the exam, wash your skin with your usual soap. There is no need to shave.
“During the infiltration, the patient, awake and conscious, is lying or sitting on an examination table. After cleaning the skin, the needle is placed following the anatomical or radiological landmarks. A local anesthetic or a Contrast material may be used depending on the technique used. The procedure is short and lasts approximately 15 minutes, after which the patient can get up and walk.”, describes the specialist. This procedure does not require fasting. On the other hand, it is advisable to be accompanied and not to drive to leave after the infiltration.
Is it painful?
The infiltration, in itself, can be painful. “Analgesic techniques can be offered depending on the practitioners’ habits (sedative treatment, hypnosis, virtual reality headset, etc.) but most of the time they are not necessary. After the injection, pain around the injection site may appear and persist for a few hours: however, taking an analgesic can relieve it.
What are the post-operative instructions?
Infiltration is a common procedure, mostly well supported. However, the occurrence of intense headaches, violent and unusual pain (at the puncture site) or a fever should lead you to contact your doctor as quickly as possible. In the event of a neurological disorder such as loss of strength or sphincter disorders (loss of urine, etc.), you must quickly consult the emergency room.
What rest after a lumbar infiltration?
Relative rest of 24 to 48 hours is suggested. Everyday activities can be carried out but it is strongly recommended to postpone intense physical activities.
What should you expect after infiltration?
The effectiveness of lumbar infiltration may not be immediate: most often, it takes a few days to obtain the desired effect.
Side effects: are there any potential complications?
Infiltration is a minimally invasive procedure, mostly well tolerated, with rare complications.
“The most severe are neurological complications following the formation of a hematoma or spinal cord ischemia phenomenareports Dr. Gilles Avenel. Fortunately, they are exceptional but the occurrence of neurological signs in the lower limbs or pelvis must lead to emergency treatment.
Spinal infections are also exceptional and are suspected when there is an increase or change in pain, especially if there is a fever. It will then be necessary to quickly carry out imaging to confirm the infection, organize hospitalization for the taking of bacteriological samples and begin antibiotic therapy.
“Exceptionally, during the injection, a dural breach may occur when positioning the needle, causing headaches which can last a few days.”
In the hours and days following the injection, the following are sometimes observed:
- Severe lower back pain or pain at the puncture site; bleeding, as well as hematoma (although rare);
- An allergic reaction to the contrast product;
- A vagal discomfort, benign and transient…
