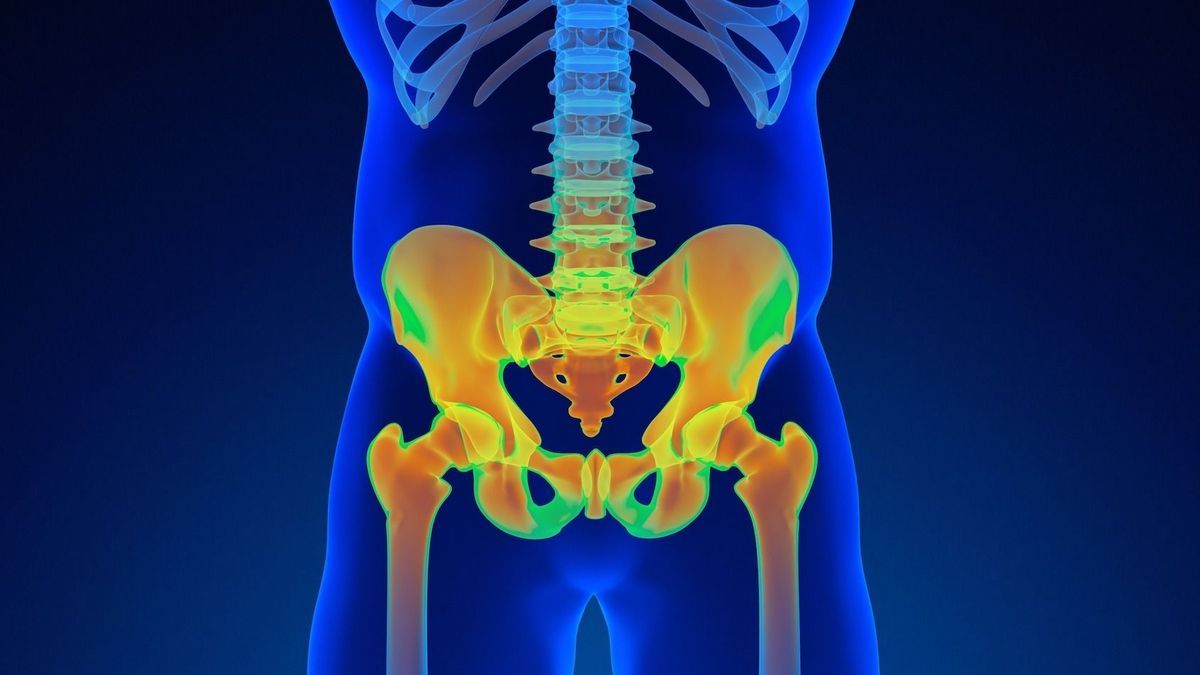
This bony pelvis has multiple functions. What are they and what are the pathologies that can alter it? The answers of Thomas Geraci, physiotherapist at the Parc clinic in Castelnau-le-Lez
Like any bone structure, the pelvis can be the site of various pains and conditions in a person. What is the right attitude to take, who to consult, what tests will help identify the cause of the pain and treat it? What are the treatments? Should we stay in our chair or encourage the continuation of activities at all costs? Fetour on the definition, pathologies and treatments with our expert.
The anatomy of the pelvic girdle
The pelvic girdle forms the bony pelvis. It is made up of three structures:
- The sacred which is the continuity of the vertebral column, with the coxal bone at the end (“coxal” means “relative to the hip”);
- THE two iliacs, these are the bones that we feel on each side of the hips. The whole forms the sacroiliac joint or SI joint;
- At the front we observe the pubic branch and the ischial branch which, joining together, forms the symphysis. This joint can be painful during pregnancy.
The functions and properties of the pelvic girdle
The pelvic girdle transmits the weight of a person’s upper body to the lower extremities. This belt also has a function of supporting and maintaining the viscera (stomach, liver, kidneys, spleen, intestines, uterus, etc.), which helps preserve them.
The pelvis is also a zone of muscular and ligamentous insertion. This is where most of the tendons and muscles are inserted to provide good support to the body. “We thus find the ligament around which is located in the pelvis at the level of the acetabulum, tells us Thomas Geraci, physiotherapist at the Parc clinic in Castelnau-le-Lez. “At the level of the legs we find the hamstrings, the gluteus medius, the sartorius (satorius muscle). At the level of the abdominals, the upper part of the body, we find the quadratus lumborum.
Pathologies associated with the pelvic girdle
There are various pathologies affecting the pelvic girdle that can affect a person’s health:
- Rheumatic diseases (ankylosing spondylitis, rheumatoid arthritis). Repetitive friction due to age or the practice of a violent sport (rugby for example) can create rheumatic pain in a person and over time alter the quality of the cartilage. The medical origin can also be bacterial. “A bacteria can settle on the bones of the pelvis and then cause inflammationpoints out the specialist. In this case, research will be focused on this bacteria in order to be able to treat it as best as possible with specific treatments. Joint pain is felt at the level of the sacrum towards the buttocks, particularly when the person bends down or sits down. “There is a time for the joints to heat up when the person starts to move.” adds the physiotherapist;
- Pelvic fracture. It can occur following a simple fall (in the bath, on the stairs, from a swing, from a bicycle, etc.). It may be a fracture of the pubic symphysis, the sacroiliac, the iliac, etc. “Fractures of the pelvis are quite common among elderly people prone to loss of balance”, indicates the specialist. In case of sacroiliac fracture, stabbing pain occurs in the hips. If it is a fracture of the ischium, the pain is located lower in the buttocks. The pain increases each time the person tries to move the leg. If the fracture occurs at the level of the pubic symphysis, the stabbing pain occurs more in front and is medically identifiable upon palpation of the area;
- Pelvic malformation. The joint from birth does not move properly. “The cartilage of the pelvic girdle then wears out more quickly causing a health problem in adulthood such as osteoarthritis due to repeated friction, indicates the specialist. Cartilage wear can also cause compensation in other joints and cause pain. If the patient cannot cope with the pain, the treatment consists of resorting to surgery to correct the location of the pelvic bones. Generally, we talk about pelvic osteotomy, an operation that involves replacing the bones of the pelvis correctly in their proper alignment.”.
What are the medical treatments depending on the pathology?
Treatment of the fracture consists of immobilizing the person, which involves changing their lifestyle habits. Thanks to these temporary changes, the person can expect a reduction in the intensity of the pain and a return to normal life within a few weeks. This requires respecting the medical advice of doctors. The patient should walk as little as possible, avoiding putting pressure on the leg on the fractured side. He will have to walk on a hopping block or use a walker or wheelchair.
If it is an elderly person predisposed to imbalance, it is recommended to stay in bed so as not to risk another fall. It is advisable not to take unnecessary risks by wanting to take a bath at all costs, for example. However, it is recommended to enjoy the comfort of your chair during the day in order to continue moving and avoid pressure sores. Don’t hesitate to get help to move from bed to chair and from chair to bed.
Allow between 4 to 6 weeks of convalescence for bone repair. The subject may be hospitalized depending on the location of the fracture and their age. “This is the case of the fracture of the iliopubic branch which does not always require surgery but rather comfort by prioritizing rest while it consolidates correctly. gives the example of the expert. “Be careful, resting does not mean doing nothing, however, you should not exaggerate your steps and avoid moving too much on your legs”. This fracture does not require any bandaging. The care also includes the administration ofAINS (Nonsteroidal anti-inflammatories) which may be prescribed to relieve pain and inflammation.
In cases of rheumatic disease, the breakdown of cartilage leads to reduced mobility. This is why muscle strengthening is fundamental to maintaining good muscle tone in the pelvic girdle. “The best treatment is to strengthen the muscles surrounding the pelvis in order to minimize friction, slipping and microtrauma. confirms Thomas Geraci. “If we do not provide any care, we risk sliding towards osteoarthritis”, he warns. “Any strengthening will be suitable because the pelvic girdle is a joint in the middle of the human body”. If the pain persists despite muscular strengthening , do not hesitate to seek another opinion from another specialist.
What are the pelvic girdle examinations?
Different examinations allow the pelvic girdle to be explored:
- As a first intention after a manual clinical examination carried out by the doctor, the patient will be subjected to a radiological examination in order to check the entire pelvic girdle and rule out the fracture. “The x-ray highlights all the bony reliefs, which makes it possible to clearly localize the fracture, if there is one, or even osteoarthritis. says Thomas Geraci.
- If there is no fracture, a pelvic scan or a Pelvic ultrasound may be prescribed in order to highlight the inflammation and at the same time to have a detailed image of the bone, ligamentous and visceral structure.
- The scintigraphy is known in particular for detecting bone metastases in the case of cancer. L’osteodensitometry checks the condition of the bones and establishes the diagnosis of osteoprosis, which makes it possible to identify people at higher risk of fractures.
Whatever your age, it is therefore important to take care of your pelvic girdle in the event of trauma or older pathology. Changing your habits for a while, changing your lifestyle, putting in place care systems will allow bones, joints and tissues to quickly regain their function and their full capacity to function normally.
