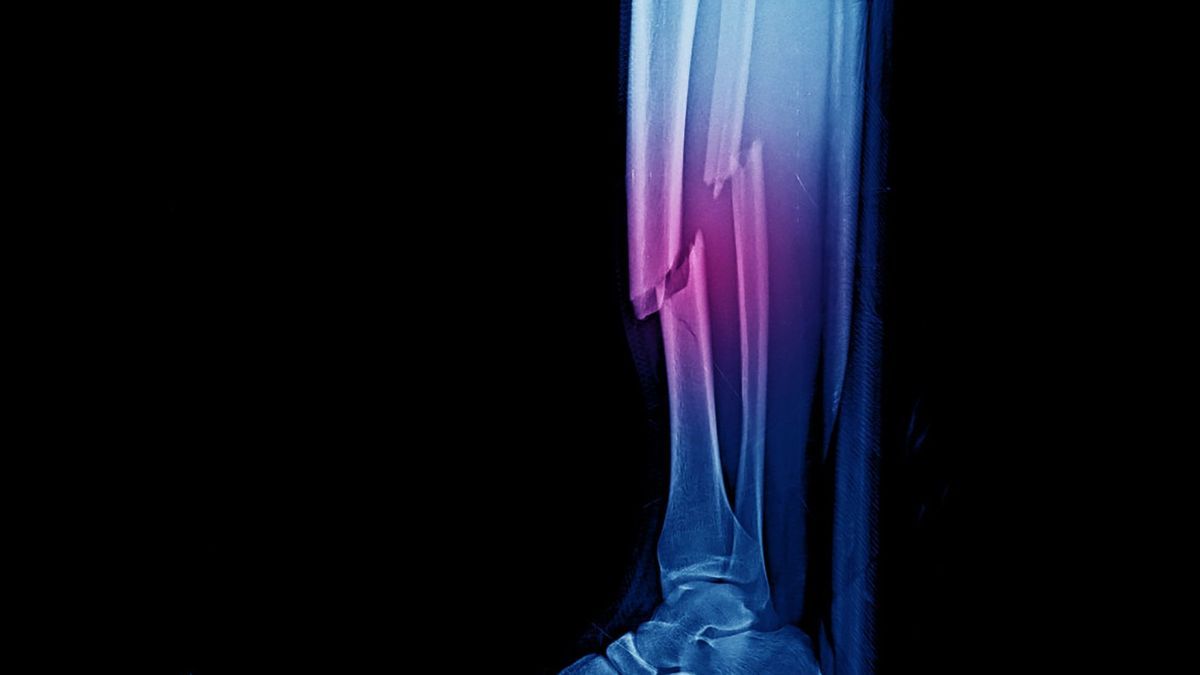
The diaphysis, or bony body, the middle part of a long bone: it concerns the femur, the tibia, the humerus, the radius and the ulna. Very resistant, it can however be fractured during violent trauma (shock during a road accident in particular) or in the event of bone disease (osteoporosis). Fracture of the femoral shaft can occur in particular in older people, whose bones are more fragile. Dr. Gilles Avenel, rheumatologist at Rouen University Hospital (Rouennais Spine Institute) and president of the Spine section of the French Society of Rheumatology (SFR), tells us more.
Anatomy, physiology: what is the diaphysis?
The diaphysis, also bony body or body of the bone, is the median, longitudinal and cylindrical, tube-shaped part of a long bone such as: the tibia, the femur, the fibula, the humerus, the radius or the ulna (or ulna). Its two ends are called the epiphyses and are covered with articular cartilage.
Between the diaphysis and the epiphysis is the “metaphysis”: in this transition zone, the diameter of the bone gradually increases as it grows.
Inside the diaphysis circulates the central medullary canal, also known as the medullary cavity. This conduit contains the bone marrow. These are the nourishing vessels which vascularize the diaphysis and the marrow in its center by forming an internal blood system, which arrives from the Volkman canals.
The diaphysis does not have cartilage. It is made up of thick compact tissue, called cortex or cortex, and is surrounded by a membrane (the periosteum), rich in nourishing vessels which participate in ossification in thickness. It is organized into very dense, longitudinal bony sections, formed of concentric columns where calcium is fixed. Ossification of the diaphysis takes place during the 3rd month of embryonic life.
The growth and maturation of bone is regulated by a hormone secreted by the pituitary gland (pituitary gland). At a certain stage, however, hormones secreted by the testicles in men and by the ovaries in women stop bone growth: the epiphyses then fuse to the diaphysis. From this moment, which generally occurs earlier in women, the bone undergoes constant remodeling (it is continually resorbed and rebuilt). The natural rebuilding of bone slows down over the years, which explains why fractures heal much more slowly in older people.
“Generally speaking, the diaphysis is the strongest and most resistant part of the bone, both in torsion and in flexion (it can support up to 280 kilos), but it can suffer trauma in the event of crushing”explains Dr. Gilles Avenel, rheumatologist at Rouen University Hospital (Rouennais Spine Institute) and president of the Spine section of the French Society of Rheumatology (SFR).
What are the pathologies that can affect it?
Several types of pathologies can affect the diaphysis:
- Bone fractures
- Bone tumors
- Bone diseases, such as osteomalacia, which cause bones to curve due to softening of their structure. Or Camurati disease which is characterized by localized sclerosis of the diaphysis.
“Fracture is the most common pathology of the diaphysis. It follows a violent shock, and mainly affects young men, victims of a violent direct shock (generally during a motor vehicle accident or a car-pedestrian collision). When it occurs without shock or for a minimal shock, it should raise suspicion of a contributing pathology such as a bone tumor.continues the specialist.
What are the treatments ?
Treatments depend on the pathology and the anatomical location of the problem.
In case of fracture
When it comes to a fracture, immobilization is necessary. Indeed, if the bone fragments consolidate in a bad position, the patient may subsequently experience after-effect pain or deformation of the limb likely to lead to other pathologies (secondary osteoarthritis, etc.). It will therefore be necessary to reduce the fracture (align the 2 parts of the bone) then immobilize them until a sufficiently solid bone callus is formed. The reduction can be carried out under simple sedation but sometimes requires general anesthesia. Immobilization can be orthopedic (by plaster or resin splint) or surgical (osteosynthesis).
In case of tumor
Depending on the nature of the tumor, specific treatment may be offered. This treatment must be discussed at a consultation meeting in order to establish the optimal treatment which can combine surgery, radiotherapy and drug treatment.
In case of bone disease
Osteomalacia
The treatment of this pathology is primarily based on prevention. A daily calcium intake helps avoid a deficit: the normal diet must include a sufficient calcium intake (dairy products, mineral waters rich in calcium). Vitamin D supplementation is also necessary and treatment with vitamin D is systematically offered to children as well as to people at risk of deficiency (little sun exposure).
Camurati disease
This is an extremely rare constitutional disease. There is no specific treatment for this pathology.
How to recognize the fracture?
The fracture of a shaft is very painful and causes significant functional impotence. The fracture also generates edema and deformity. A hemorrhagic syndrome which can lead to hemorrhagic shock can occur, particularly if the fracture affects a large bone and it occurs in a context of polytrauma.
How to make the diagnosis?
Imaging, most often an x-ray, front and side, allows the diagnosis to be made. Sometimes a CT scan may be necessary.
How to reduce the divide?
Immediate treatment involves placing a femoral traction splint (such as a Hare or Sager traction splint) before surgery. However, it should not be used if the patient also has a tibial fracture.
- Cast immobilization : it is mainly reserved for children and non-displaced fractures. Prolonged immobilization carries a risk of secondary displacement of the fracture and is unsuitable for a femur and humerus. This type of treatment requires regular radiological monitoring;
- Traction treatment : it consists of traction in the axis of the limb via a pin or a system of glued bands. However, it is most often a waiting treatment, before surgical treatment and linked to different reasons (medical, equipment not available, need for authorization by the guardianship, etc.);
- Bloody reduction with internal osteosynthesis : internal osteosynthesis (repair and fixation of the bone) is the most frequently used operating technique. The procedure takes place under general anesthesia and under fluoroscopic control. Several incisions are made on the external face of the thigh at the top and bottom, in order to introduce the fixing material (femoral nail, plates, etc. fixed by screws) into the bone and maintain the fracture. The surgeon uses a femoral nail which he will introduce into the bone or one or even several plates. Once the operation is completed, the skin is closed.
What instructions after the intervention?
The pain can be significant, but it subsides after 72 hours after the operation. Hospitalization lasts a few days, then the patient can return home or to a care and rehabilitation center with canes or crutches (if support is authorized).
Nursing care is required every 2 to 5 days until healing and physiotherapy is often implemented.
The duration of the work stoppage depends on the professional activity. It is estimated that driving can be resumed when the person can walk without assistance.
Furthermore, a clinical and radiographic check must be carried out with the surgeon one and a half months after the operation.
Possible complications?
Complications are possible, however they remain rare because several measures can prevent them.
- Like any surgery, there is a risk of hematoma which generally resolves on its own. Exceptionally, it may require an evacuation puncture or surgical drainage;
- Complications can occur during the procedure such as vascular and more rarely nerve damage. A new fracture may also occur after the operation and require extension of the osteosynthesis. Bone fragility (osteoporosis) is a contributing factor;
- Healing can be disrupted in particular in cases of excess weight, smoking, arterial vascular insufficiency (arteritis) or when taking certain treatments (corticosteroids in the context of inflammatory rheumatism);
- To prevent the risk of phlebitis, preventive anticoagulation is always continued until the lower limb is restored;
- Strict monitoring also prevents the risk of compartment syndrome (increase in pressure in an inextensible muscle compartment with the consequence of hyperpressure which causes muscle ischemia), of the leg or upper limb;
- Complications linked to prolonged bed rest are sometimes observed: urinary or pulmonary infection, pain, skin irritation of the heels sometimes leading to a bedsore, etc.
- A blistered and annoying scar (keloid) can form in…
