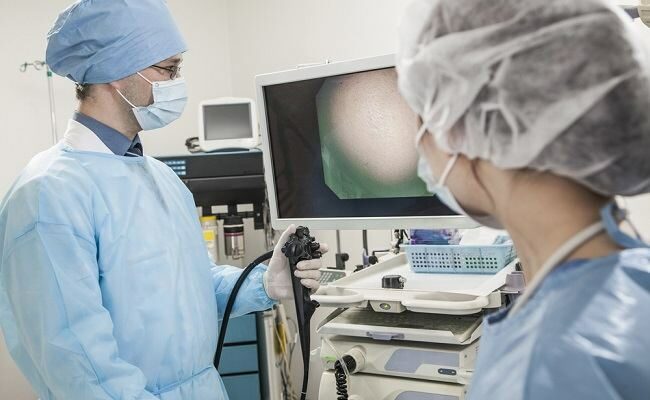
Colonoscopy is a procedure to detect injuries, irritation, polyps or cancer in the large intestine and rectum, which is the lowest part of the large intestine that is connected to the anus. This procedure is carried out preceded by the administration of anesthesia to the patient.
Colonoscopy is performed using a colonoscope, which is a flexible tube with a diameter of about 1.5 cm. This tube is equipped with a small camera at the end, which functions to send images to a monitor so the doctor can see whether there are abnormal conditions in the large intestine.
If abnormal tissue is visible during the examination, the doctor will take a tissue sample (biopsy) from the large intestine during a colonoscopy.
Colonoscopy Indications
Doctors usually recommend colonoscopy procedures for the following purposes:
- Detect colon cancer, especially in people aged 50 years and over and people at risk of developing colon cancer
- Find out the causes of bloody stools, chronic constipation, chronic diarrhea, abdominal pain, and other complaints related to the intestines
- Detects and cuts intestinal polyps, while reducing the risk of developing colon cancer
- Stops bleeding if bleeding occurs in the large intestine
Warnings Before Undergoing a Colonoscopy
Undergoing a colonoscopy procedure during pregnancy should be avoided because it can trigger miscarriage. Colonoscopy is also not recommended for people with megacolon and people with inflammation of the intestine with serious injuries, because it can increase the risk of the intestine tearing.
To prevent interference during the examination, tell your doctor if you are taking the following medicines:
- Arthritis medication
- Aspirin or other medicines that contain aspirin
- Blood thinning medication
- Diabetes medication
- Non-steroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen or naproxen
- Supplements or vitamins that contain iron
Before Colonoscopy
So that the colonoscopy examination runs smoothly, there are several things that must be prepared, namely:
Ensure the intestines are clean
Before a colonoscopy is performed, the intestine must be clean of feces (feces) so that the intestine can be seen clear and clear during the examination. For this reason, the doctor will ask you to do the following things before undergoing a colonoscopy:
- Take laxatives the evening before the colonoscopy and in the morning before the colonoscopy
- Follow a special diet by eating only soft foods and drinking water the day before the colonoscopy
- Fast after midnight before undergoing the colonoscopy procedure
- Stop or reduce the dosage of any medications you are taking, including supplements and vitamins, at least 1 week before the colonoscopy
Make sure someone is there to accompany you
Make sure that you have family or relatives to accompany and accompany you when you undergo the colonoscopy. This is because you will be under anesthesia for up to 24 hours after the colonoscopy so it is not safe to drive alone.
Colonoscopy Procedures and Actions
Before carrying out a colonoscopy, the doctor will give you an anesthetic first. In some cases, anesthesia can be combined with pain medication to reduce discomfort that may occur during the procedure.
Next, the doctor will perform a colonoscopy, the steps are as follows:
- The patient will be asked to lie facing sideways. The patient will also be asked to bend his knees in front of his chest.
- The doctor will insert the colonoscope into the patient’s rectum and push it down to the large intestine. During this process, the camera will send images to a monitor so the doctor can see the condition of the colon.
- Once the tip of the colonoscope reaches the large intestine, air will be blown through the tube so that the patient’s intestine expands and the intestinal wall is clearly visible on the monitor. At this stage, the patient will feel a slight cramp, but it can be relieved by taking a deep breath.
- Once the tip of the colonoscope reaches the opening of the small intestine, the colonoscope will be slowly withdrawn. At this stage, the doctor will examine the colon once again.
- If necessary, the doctor can insert a special tool through the colonoscope. This process is carried out to take tissue samples from the intestine (biopsy), remove polyps, or remove other abnormal tissue from the intestine.
The entire colonoscopy procedure generally lasts around 30ꟷ60 minutes. If the quality of the image produced during a colonoscopy is deemed unclear, the doctor can repeat the procedure.
If there is a part of the intestine that the colonoscope cannot reach, the doctor will perform an X-ray examination with the help of barium fluid (virtual colonoscopy).
After Colonoscopy
After the colonoscopy procedure, the patient must remain in the treatment room for 1–2 hours or until the effect of the anesthetic wears off. The patient may feel bloating and cramps in the stomach, but these complaints will subside on their own.
Colonoscopy results are declared positive if the doctor finds polyps or abnormal tissue in the intestine. In such conditions, the doctor will examine the tissue sample in the laboratory.
On the other hand, the results of a colonoscopy are declared negative if the doctor finds no abnormal conditions. Even so, doctors can recommend that patients undergo a colonoscopy again in the next 5ꟷ10 years, if there is a risk of colon cancer.
There are several conditions where doctors recommend that a repeat colonoscopy be performed, namely:
- There is residual feces in the intestine, blocking the view of the camera during a colonoscopy
- More than one polyp is found or the polyp is suspected to be at risk of developing into cancer
- The diameter of the polyp is more than 1 cm
- Polyps are cancerous
Other things to pay attention to after undergoing this procedure are:
- Do not drive or do activities that require alertness until 1 day after the colonoscopy
- Consult with your doctor about the right time to resume taking medication that has been temporarily stopped
- Follow your usual diet after a colonoscopy, unless your doctor advises otherwise
If a colonoscopy is followed by polyp removal or biopsy, light bleeding from the rectum may occur for 1-2 days, but this is normal.
When to see a doctor
You are advised to immediately seek medical help if the following complaints appear after undergoing a colonoscopy:
- Dizzy
- Weak
- Fever
- Severe stomach pain
- Having bloody stools that don’t go away for more than 1 day
Bleeding from the anus that doesn’t stop
Colonoscopy Side Effects
In general, colonoscopy is a safe procedure. However, in rare cases, colonoscopy can cause the following side effects:
- Bleeding
- Severe stomach pain
- Allergic reactions and side effects of anesthetic drugs
- Perforation or tear in the colon wall